Scientific Research
The results are impressive: One year after the surgery, 91% of the patients questioned were “very satisfied” or “satisfied” with their knee joint prosthesis. Two years after the surgery, 88% of the patients are “very satisfied” or “satisfied”. Almost all patients (96%) would have the surgery performed again under the same circumstances. In addition, 88% of patients after one year and 89% after two years state that the condition of their knee joint is “very much better” or “significantly better” than before the operation.
Our patients’ functional ability also improved significantly in the first two years with the “new” knee joint. The following diagram provides an overview:
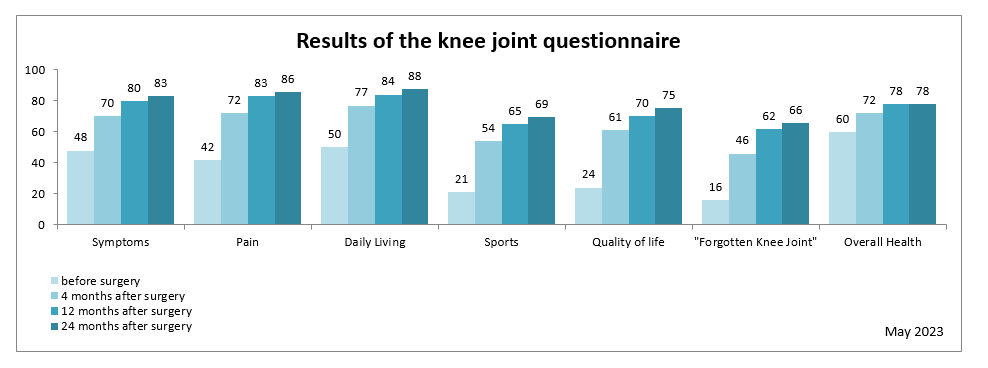
The scale is from 0 to 100 points with higher values indicating better function.
The figure tells you, that knee function measured in different subscales clearly improved four months after the surgery and still increases over the next months. Likewise, the overall health state that not only refers to the knee could be improved. The term “forgotten knee joint” means, that you are not aware of your artificial knee joint in everyday life. It indicates how normal your knee joint feels.
To collect so called „patient-reported outcome measures“ (PROMs) means some extra effort for us, especially as we are interested in long term results. This project is all the more important because it reflects the patient’s perspective and gives us valuable information about the success of therapy. The participation is of course voluntary. Approximately 80% of our patients agreed to complete six questionnaires in five years. The high number of participating patients gives even more importance to our very good results.
For more information please click here: https://leonardo-ortho.ch/en/practice/scientific-research/