- Home
- Flat Foot Pes Planovalgus
Flat Foot Pes Planovalgus
DEFINITION/DEVELOPMENT
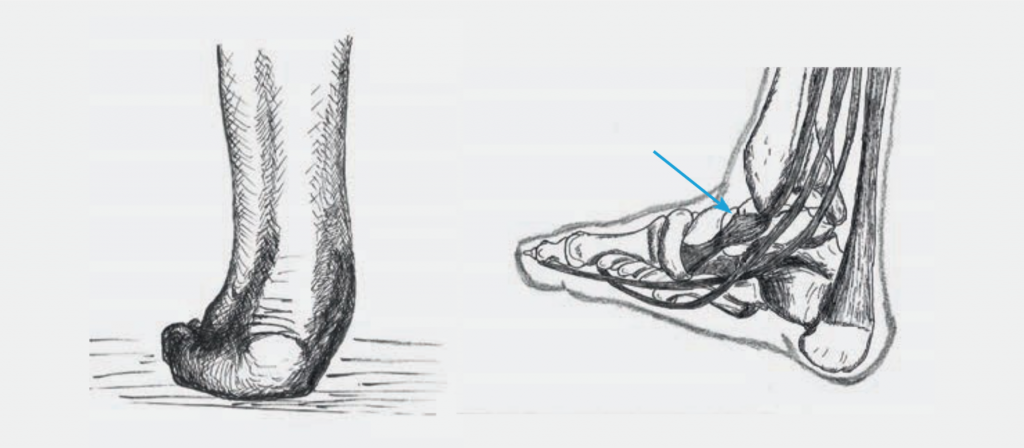
A flat foot (Fig.1) can have various causes. There are essentially two types of flat feet. On the one hand congenital, on the other hand the acquired flat foot.
There are mild forms of congenital flat foot, which belong to the normal range of different foot shapes. The more pronounced flat foot deformities have some skeletal changes. These include the coalition and the accessory navicular bone (Os tibiale externum). Coalition is the connection of the bones in the foot, so that the joint between these connected bones is rigid rather than mobile. The subtalar (lower ankle) joint is most frequently affected. The accessory navicular bone is an additional bone nucleus that does not fuse with the navicular bone during growth. It is located where an important tendon (posterior tibial tendon) begins to support the arch of the foot.
The acquired flat foot is not primarily a skeletal deformity but a change in the tibialis posterior tendon that supports the arch of the foot. Here, inflammation and degenerative changes of the tendon can occur with age. Pain develops and with time the tendon becomes weaker and can no longer hold the arch of the foot. This results in the development of a flat foot and the foot increasingly looks outwards. At first this malposition is still flexible/reversible, but with time it becomes fixed and is no longer reversible.
SYMPTOMS
Most patients with a congenital flat foot have no problems. With coalition, pain usually only occurs over time. Since the lack of mobility of the subtaler joint is compensated, the ankle joint is often very mobile or even unstable. Patients report frequent sprains since their youth. The accessory navicular bone does not usually cause any complaints either. Occasionally, however, persistent pain and swelling can occur in this area (inside of the foot), especially after an accident or a violent blow.
In the case of an acquired flat foot (Fig. 2), there may be pain and swelling on the inner edge of the foot. On the other hand, patients usually also notice a change in the shape and position of the foot (increase in bending, foot looks more outwards). The cause is a weakness of the posterior tibial tendon. Over time, the arch of the foot can no longer be stabilized, and a one-legged tip-toe is no longer possible.
EXAMINATION
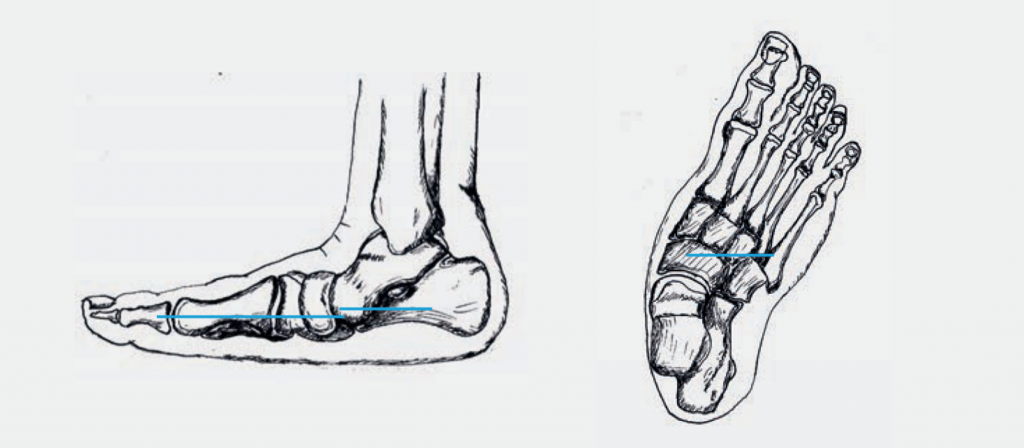
During the examination, the malposition is visible and it must be assessed whether it is a fixed or flexible malposition. Pressure points are sought and the strength of the tendon is checked. The mobility of the joints and any instabilities are also examined.
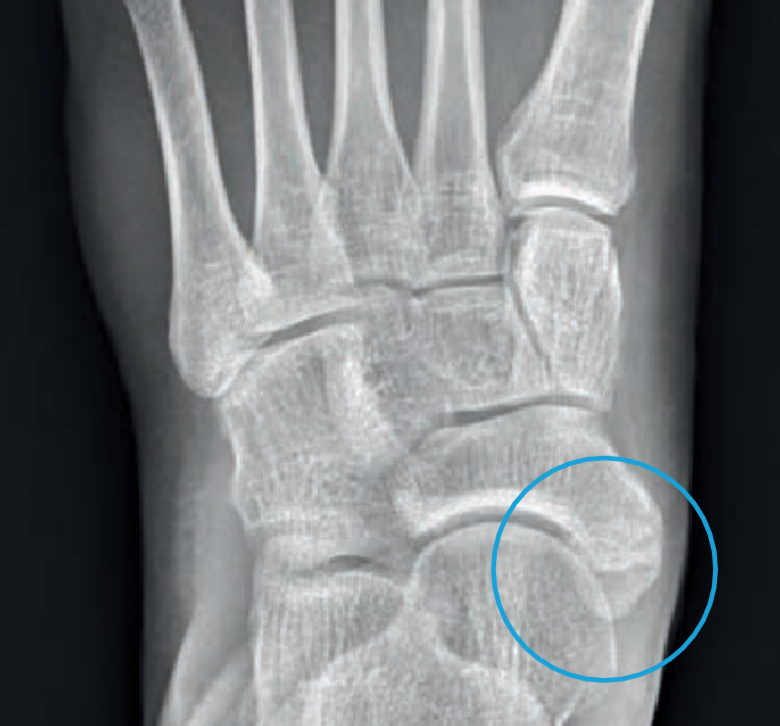
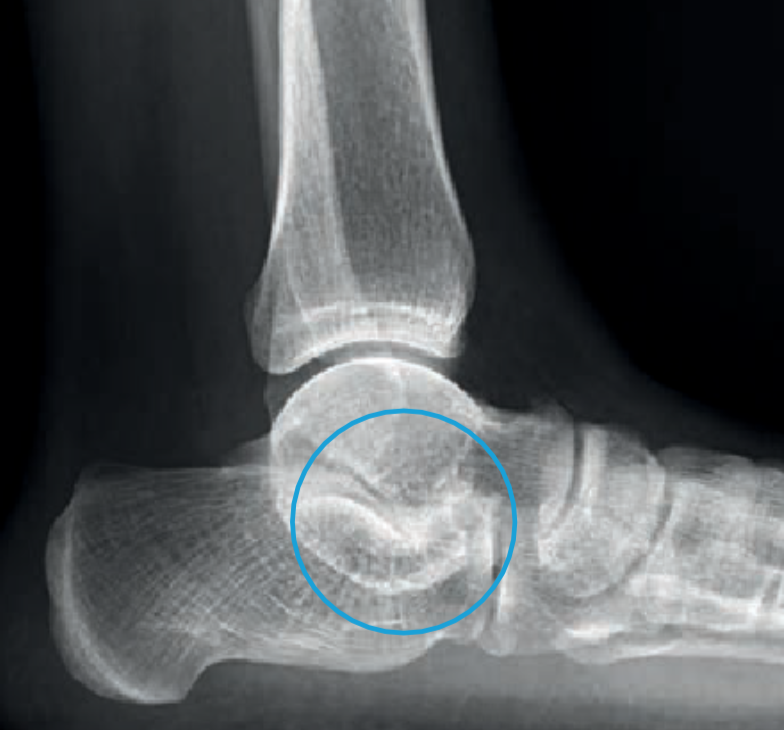
The first examination includes strained x-rays. There the foot position can be assessed. Additional bone nuclei are displayed (Fig. 3) and sometimes a coalition (Fig. 4) is already visible. Depending on the situation, additional examinations make sense. An MRI shows tendons better and a SPECT/CT, for example, a painful accessory navicular bone.
TREATMENT
Because of the many different causes and forms of a flat foot, the therapies are also very different.
A) Non Surgical
Congenital flat feet do not need to be treated as long as they do not cause complaints. Even if there is a coalition or an accessory navicular bone, treatment is only necessary if there are complaints. If the complaints are only minor, insoles can be adjusted as a first treatment. In the early stages of an acquired flat foot, an improvement can also be achieved by adjusting insoles and physiotherapy.
B) Surgical
Depending on the situation, the following operations are possible:
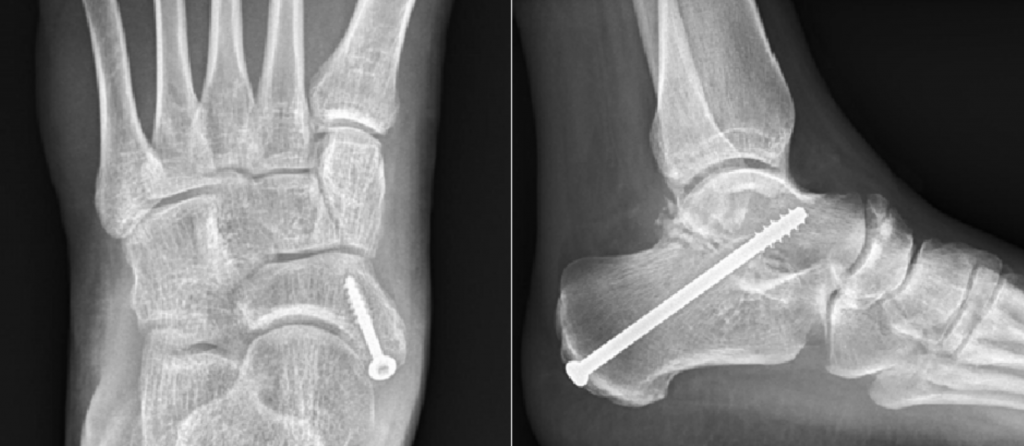
1. In the case of a painful accessory navicular bone, this cannot simply be removed, as otherwise the tendon attachment is injured, and the tendon is subsequently weakened. Therefore, the additional bone fragment must be fixed to the navicular with a screw (Fig. 5 left).
2. Removing of the coalition with mostly subsequent fusing in corrected position (Fig.5 right):
Adhesions between the bones can be loosened or chiseled up. Thus, a joint is created again. However, since it is not covered with cartilage and this joint has never been moved, it usually has to be fused. This involves correcting and straightening the position of the hindfoot bones. This way the pain can be treated, and a functionally good position can be achieved.
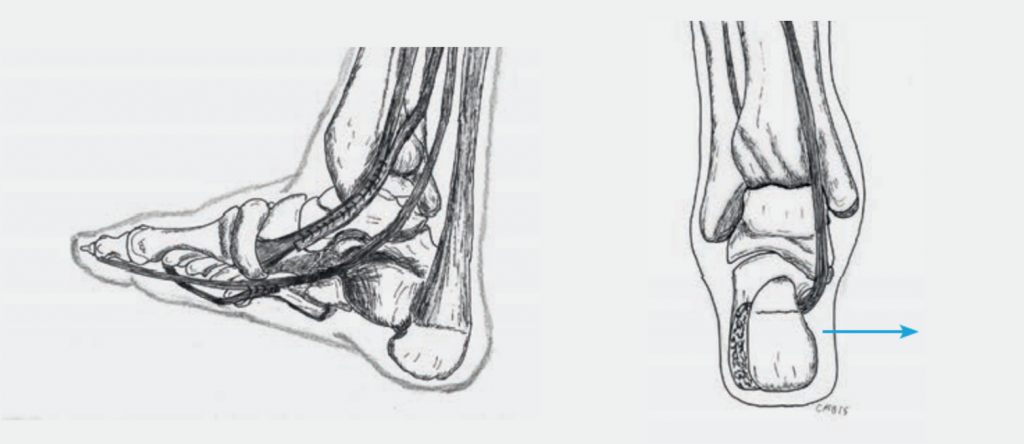
3. Tendon Transfer and correction of heel position (Fig.6):
In the case of flexible acquired flat foot, a tendon transfer of the toe flexor is used to reinforce the weakened posterior tibial tendon. At the same time, the tendon is relieved with a slight inward displacement of the heel. This procedure gives good results in terms of pain, even if the flat foot position reoccurs in part.
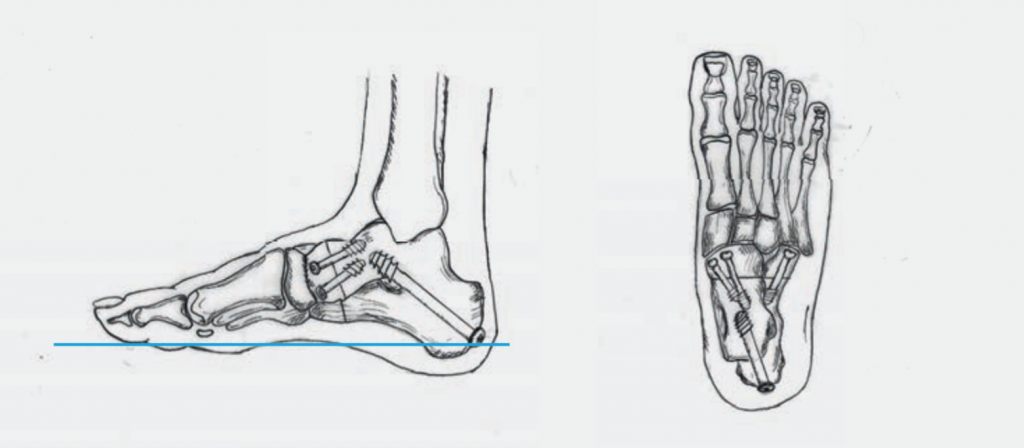
4. Fusion (stiffening) of joints to correct a fixed/rigid flat foot positon (Fig.7):
In the case of fixed/rigid flat foot, corrections are only possible directly on the bone. A tendon transfer is of no use anymore because the joints are already stiff. These joints are therefore corrected and surgically fused in a functionally better position. This does not change the mobility, but the pain and function improve due to the better position of the foot. To fix the joints in a good position, various screws must be inserted. These usually do not have to be removed.
RISKS AND COMPLICATIONS
Complications and risks may occur during or after the operation and delay the healing process or make further surgery necessary. They can never be completely ruled out during surgery, even if they are rare during foot surgery. These are summarized below:
- Wound healing disorders
- Infections
- Vascular injuries, secondary bleeding, bruising, blood loss – Nerve injuries
- Non Union (lack of bone healing)
- Interfering implants (screws, plates)
- Thrombosis, embolism
- Residual complaints
- Residual malalignment
FOLLOW UP TREATMENT
The operation is only a part of the whole treatment. The post-operative treatment plays a major role in the success of the operation. It is important that you know what you should observe and possibly avoid.
Dressing and Wound Care
During the time in the hospital you will be shown how to take care for the wound. As long as the wound is not completely dry (wound secretion/blood), the dressing should be changed daily. Do not use ointments or powders directly on the wound surface until the stitches have been removed! Disinfection is not necessary. Always remove the entire dressing when changing. The new dressing must be dry and must not slip.
If the wound is dry, a normal plaster (quick bandage) is sufficient. An elastic bandage can protect and cushion the operated area a little. The remaining swelling is also reduced. If you are not sure whether everything is normal, you can contact your family doctor or contact us directly.
The stitches can be removed about 2 weeks after the operation, usually by the family doctor. If you have a cast, the stitches can be removed during a cast change at our clinic. This can also be done 6 weeks after the operation.
Swelling and Pain
After an operation the affected foot is always more or less swollen. This swelling can occur repeatedly over weeks (up to 6 months). The most effective measure to prevent this is to elevate the leg. It makes sense to move several times a day (walking, less standing), but only for a short time. If the foot is strained and starts to hurt, this is a sign to elevate the leg again.
It is important to know that there is a general tendency for the foot to swell after foot surgery. This reaction is normal and disappears again after 6 to 12 months.
Despite these measures, pain in the operated foot can occur in the first days and weeks after the surgery. However, to relieve the pain, you can take the pain medication prescribed to you.
Weight-Bearing
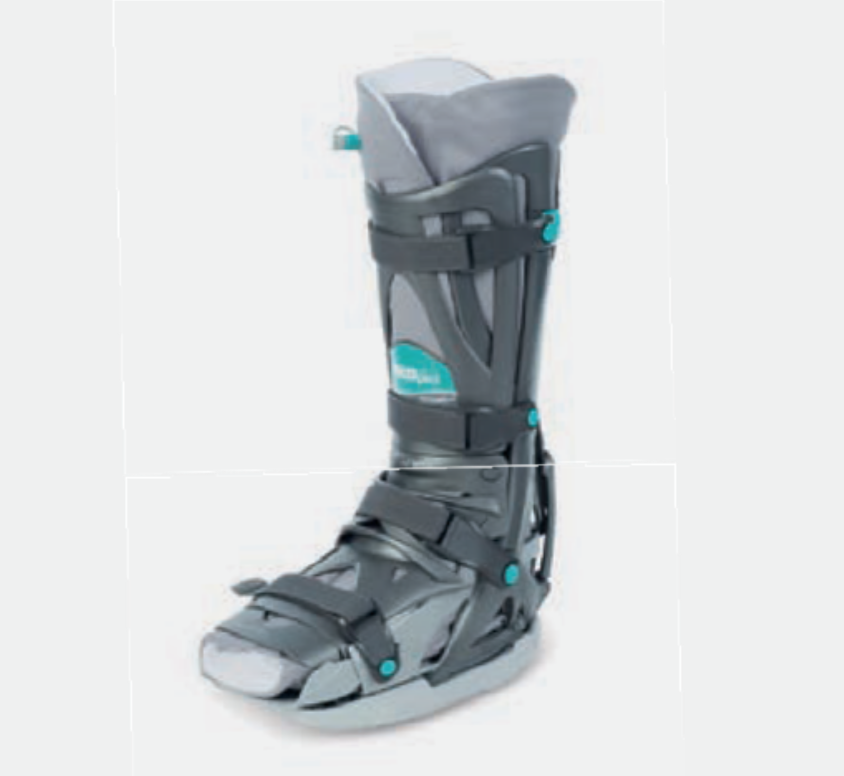
The permitted weight-bearing on the foot depends on the operation performed. To protect and facilitate mobility, you have been given a special shoe (Fig. 8) or a plaster cast. As a rule, a partial weight bearing of 15 kg is recommended.
Partial Weight-Bearing
You can put about 15 kg of weight on the affected foot. This corresponds approximately to the weight of the leg and means that you must always use the crutches. To be able to do this correctly, you will be instructed by our physiotherapists. It is important that you are able to take a few steps on the stairs on your own with the crutches. The partial weight-bearing capacity must be maintained until the first follow-up check with us approx. 6 weeks after the operation.
Personal Hygiene
As long as the stitches are still in the wound, i.e. usually in the first 2 weeks, the operated foot should be protected with a plastic bag. The easiest way is to pull the plastic bag over the special shoe. As soon as the stitches are removed, you can shower and bathe without further precautions. If you have received a cast, you should protect it from water with a plastic bag.
Thrombosis Prophylaxis
Thrombosis prophylaxis already begins during the hospital stay. Depending on the operation, this prophylaxis must be continued. In most cases we use Fragmin 5000 IE ready-to-use syringes. They are administered once a day by the patient himself. You will be instructed by our nursing staff during your stay.
How long the injections have to be administered depends on the operation and the individual risks and is necessary until the patient is fully weight bearing or walking without crutches. This usually means 6-8 weeks.
Work Ability
A rest period is crucial after an operation. In the first 2 weeks you should take it easy and not work. How long you will be completely unable to work depends on the type of operation as well as your stress profile. In most cases you and your employer should be able to temporarily find less stressful work. This enables early resumption of work.
The signed work absence that you will receive from us is a preliminary assessment. The certificate can be extended if you are not able to resume work after this time. If this is the case, report to your family doctor or to us.
However, you may take up your work again any time before the given date, if you feel capable to do so.
Driving a Car
At what point you can resume driving again depends on the kind of operation you had. You must refrain from driving as long as you cannot fully weight bear your foot or are still requiring crutches. How far thereafter your ability to drive is restored is up to you. In case of doubt or if you are unsure, we recommend that you avoid driving.
Check-Ups
Six weeks after the operation, your surgeon will carry out a check-up (depending on the operation performed with x-rays). Afterwards the further procedure will be determined.
About three months after the operation, most everyday activities can be resumed. Sporting activities should only be slowly increased after 3-4 months, in order not to provoke an overuse after the sports break.
pdf for download: Flat Foot Pes Planovalgus