- Home
- Carpal Tunnel Syndrome
Carpal Tunnel Syndrome
Definition
Carpal tunnel syndrome is the most common nerve compression syndrome. The median nerve (middle nerve) innervates the skin of the thumb, index finger, middle finger and half of the ring finger and the muscles of the thenar eminence. Together with all flexor tendons, it runs through a narrow tunnel at the wrist, the carpal tunnel. This anatomical tunnel is contained at the base and the sides by the carpal bones and a strong ligament forms the roof.
Causes
An increase in the volume of the carpal tunnel (e.g. thickening of the flexor tendons due to tenosynovitis) or a decrease in volume (e.g. bruising if the radius is fractured) increases the pressure on the median nerve. Systemic diseases (e.g. diabetes mellitus) or pregnancy can also increase the likelihood of carpal tunnel syndrome.

Symptoms
As a result of the pressure increase, most patients initially complain of numbness and tingling in the thumb and index / middle finger, typically at night. Relief typically occurs after shaking hands. Over the course of time, the numbness of the fingers can also occur during the day or never disappear completely. At a very advanced stage, the muscles at the base of the thumb waste away (arrow).
Examination
If such symptoms are present, a neurologist should conduct a clinical examination and measure the nerve conduction velocity. Depending on the severity of the findings, conservative measures (night positioning splints) may initially be considered or a carpal tunnel release surgery will be recommended.
Surgical Procedure
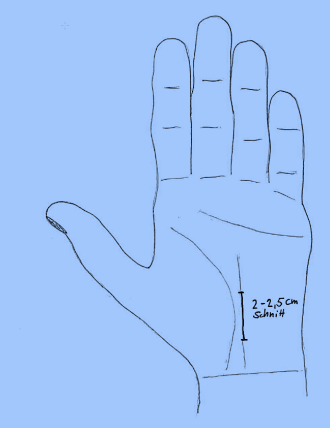
The operation is carried out under local anesthesia on an outpatient basis (exception: surgery on both hands at the same time (which usually requires 2 days in the hospital). After making a skin incision of 2-2.5 cm on the palm of the hand, the carpal tunnel is exposed with special instruments. Using a sophisticated knife that slides on a track (to protect the nerve from injury) the carpal tunnel is released. After that, only the skin is sutured. There is usually no necessity for a drain and immobilization in a splint is not required. Operating time: approx. 20 minutes.
Risks
Risk of infection: less than 1%
Likelihood of damage to relevant vessels/nerves: less than 1%
It takes about 6 weeks to regain full strength
A hyper-sensitive scar and thumb/small finger bumps: 5-10% (duration: up to ½ year)
Excessive scarring: depending on individual wound healing tendency
Follow-up Treatment
If the wound heals without complications, your family doctor can carry out regular wound checks and stitch removal 14 days after the operation. A splint is not necessary and you can begin using your hand immediately after the anesthetic induced numbness has subsided. Avoid contact with water until the wound has healed completely and weight-bearing loads (lifting heavy objects). Experience has shown, however, that already on the first day after the operation most patients report a significant reduction in the number of complaints that previously existed, e.g. can hold cutlery and get dressed without help.
